Many people think memory issues are part of aging.
But is your snoring and forgetfulness caused by age – or sleep apnea? If you feel tired and/or sleepy all the time, or if you’ve been told you snore or stop breathing during your sleep, obstructive sleep apnea (OSA) may be the cause.
But there’s good news: Forgetfulness caused by sleep apnea can be reversed!
- How does sleep apnea cause snoring?
- The surprising connection between sleep apnea and memory loss
- Are there other causes of reversible memory loss?
- Can CPAP treatment reverse brain damage?
- If I have sleep apnea, are there other benefits of CPAP treatment?
- Overcome memory problems caused by sleep apnea
- References
Listen to the article
How does sleep apnea cause snoring?
Snoring is the sound that is made when you try to breathe in while your airway is obstructed. Some people with sleep apnea may make a choking or gasping sound, while others experience silent breathing pauses as they try to inhale. The common factor is that oxygen isn’t getting through to the brain.
Here’s what happens:
- The airway becomes blocked (obstructed) during sleep, which causes a pause in breathing.
- When we stop breathing our oxygen levels drop, which triggers the brain to tell us to wake up and breathe.
- However, we don’t wake up completely (these sleep interruptions are called “micro-arousals”).
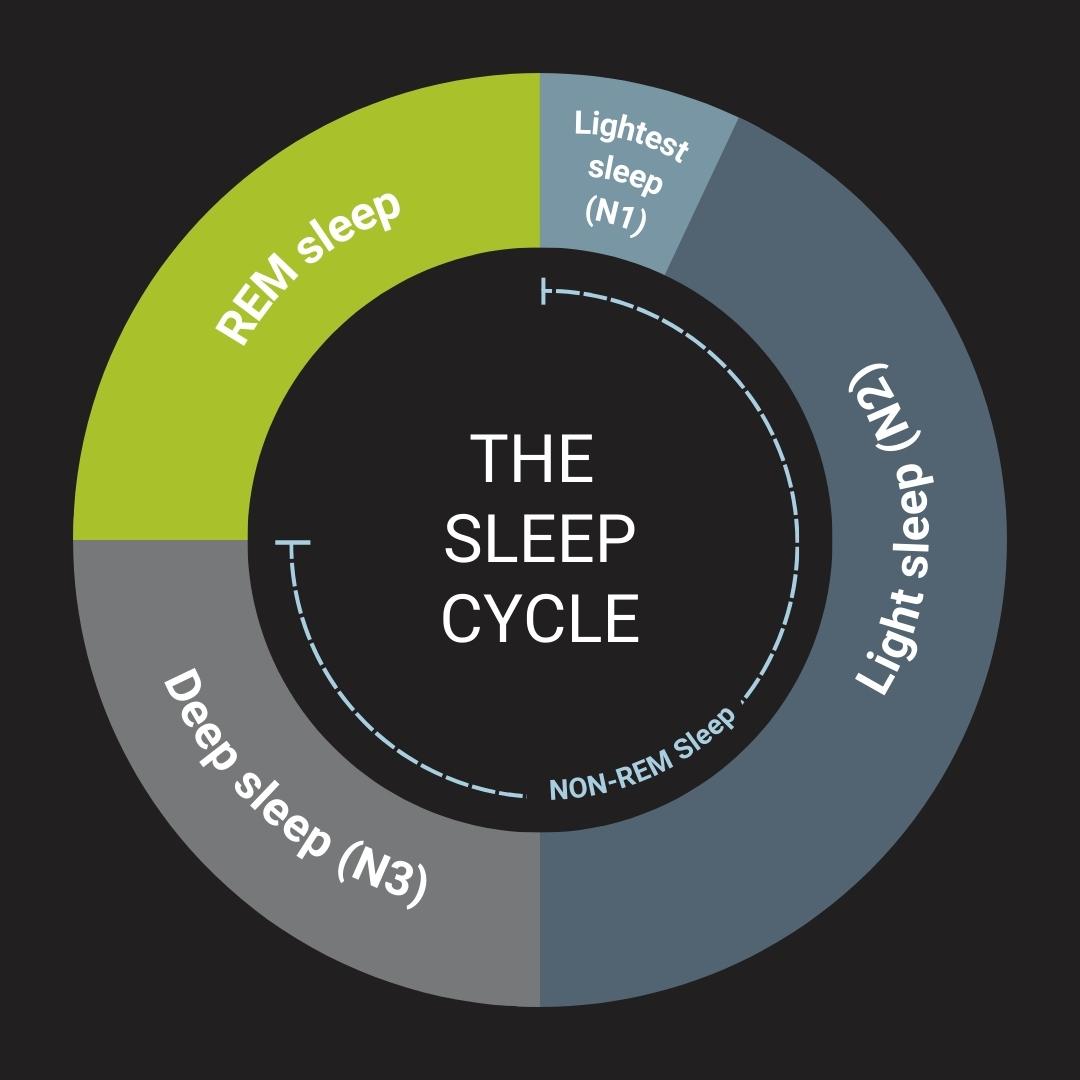
- It’s these micro-arousals that disrupt our sleep architecture and cause us to wake up in the morning feeling as if we haven’t slept a wink.

The surprising connection between sleep apnea and memory loss
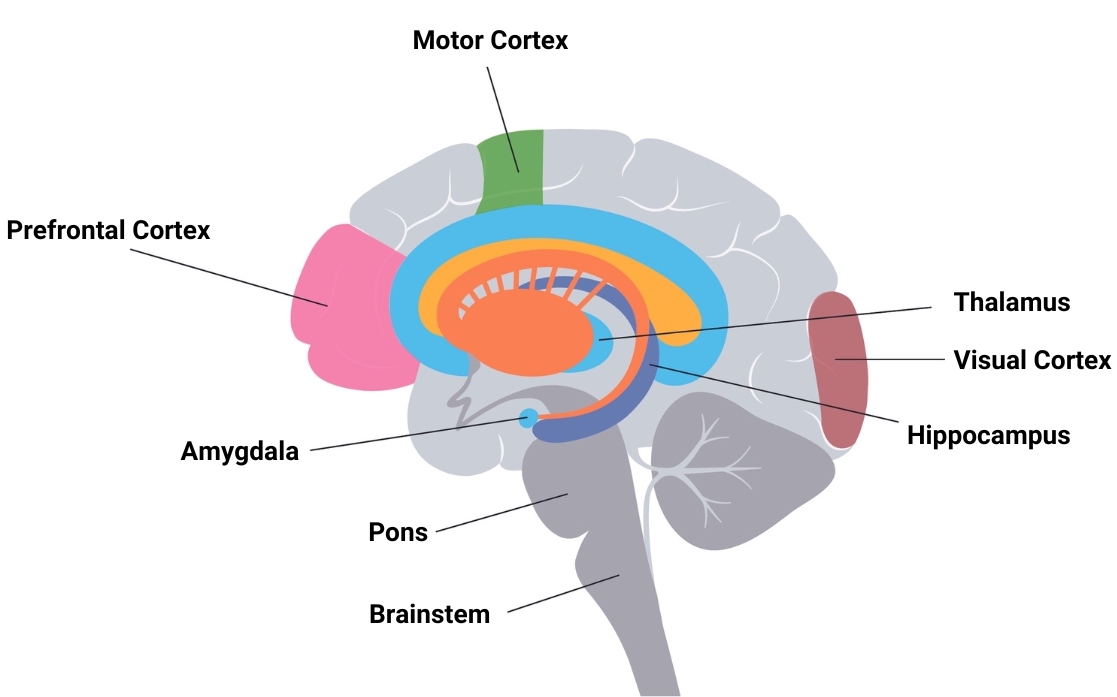
According to a study published by the American Academy of Sleep Medicine in 2017, people with severe, untreated sleep apnea had significant damage in multiple areas of the brain. In an analysis of 42 studies comparing 2294 adults with untreated OSA and 1364 adults who were healthy,¹ the authors found people with sleep apnea experienced problems with:
- Immediate recall (“What did my doctor just tell me?”)
- Delayed recall (“Who phoned this morning?”)
- Learning (“I just can’t get the hang of it!”)
- Recognition (“Right! I remember him – we met before!”)

Are there other causes of reversible memory loss?
According to the Mayo Clinic, other possible causes of reversible memory loss include:
- Medications. Certain medications or a combination of medications can cause forgetfulness or confusion.
- Minor head trauma or injury. A head injury from a fall or accident — even if you don’t lose consciousness — can cause memory problems.
- Emotional disorders. Stress, anxiety or depression can cause forgetfulness, confusion, difficulty concentrating and other problems that disrupt daily activities.
- Alcoholism. Chronic alcoholism can seriously impair mental abilities. Alcohol can also cause memory loss by interacting with medications.
- Vitamin B-12 deficiency. Vitamin B-12 helps maintain healthy nerve cells and red blood cells. A vitamin B-12 deficiency — common in older adults — can cause memory problems.
- Hypothyroidism. An underactive thyroid gland (hypothyroidism) can result in forgetfulness and other thinking problems.
- Brain diseases. A tumor or infection in the brain can cause memory problems or other dementia-like symptoms.

Can CPAP treatment reverse brain damage?
Yes! But you need to stick with the program. In the 2017 study from the American Academy of Sleep Medicine,² only limited improvements were seen after three months of treatment with CPAP. However, after just one year, CPAP therapy led to an almost complete reversal of white matter (brain) abnormalities. According to the Academy, “Treatment also produced significant improvements in nearly all cognitive tests, mood, alertness and quality of life.” All of that without medication – and with the added benefit of getting a restful night’s sleep!

If I have sleep apnea, are there other benefits of CPAP treatment?
The benefits of CPAP treatment go far beyond reversing memory loss. According to Dr. Timothy Morgenthaler², President of the American Academy of Sleep Medicine (2017), “Obstructive sleep apnea is a destructive disease that can ruin your health and increase your risk of death,” creating health hazards that include high blood pressure, heart attack, stroke, obesity and type 2 diabetes. Through treatment with CPAP, all of these hazards can be reduced. Now, that’s information worth remembering!

Overcome memory problems caused by sleep apnea
The first step is to get tested for sleep apnea.
If you have OSA symptoms and feel that your sleep is not restful, it’s important to talk to your doctor about it. Apnée Santé offers simple, fast and effective home testing. You can also contact us for a free evaluation to see if sleep testing is right for you. Here’s a checklist to review with your doctor for signs of sleep apnea.
- Loud snoring
- Occasionally waking up during the night feeling that you’re choking or gasping
- Restless sleep
- Having a sore or dry throat in the morning
- Having a headache in the morning
- Sleepiness, low energy or fatigue during the day
- Feeling sleepy behind the wheel
- Weight gain
- Erectile dysfunction
- Forgetfulness, mood changes, and a decreased interest in sex
References
- Wallace A, Bucks RS. SLEEP 2013;36(2):203-220.
- Accessed at https://aasm.org/brain-damage-caused-by-severe-sleep-apnea-is-reversible/ on Aug. 7, 2019.